-
Preventing Gum Disease in Children: Tips for Parents on Promoting Healthy Gums
Promoting Healthy Little Mouths

As parents, we strive to help our children grow up healthy and strong in every possible way. Good dental hygiene is a big part of that, not just to prevent cavities but also to reduce the risk of gum disease. It’s never too early to start promoting healthy teeth and gums. Continue reading “Preventing Gum Disease in Children: Tips for Parents on Promoting Healthy Gums”
-
Why Your Gum Line Recedes
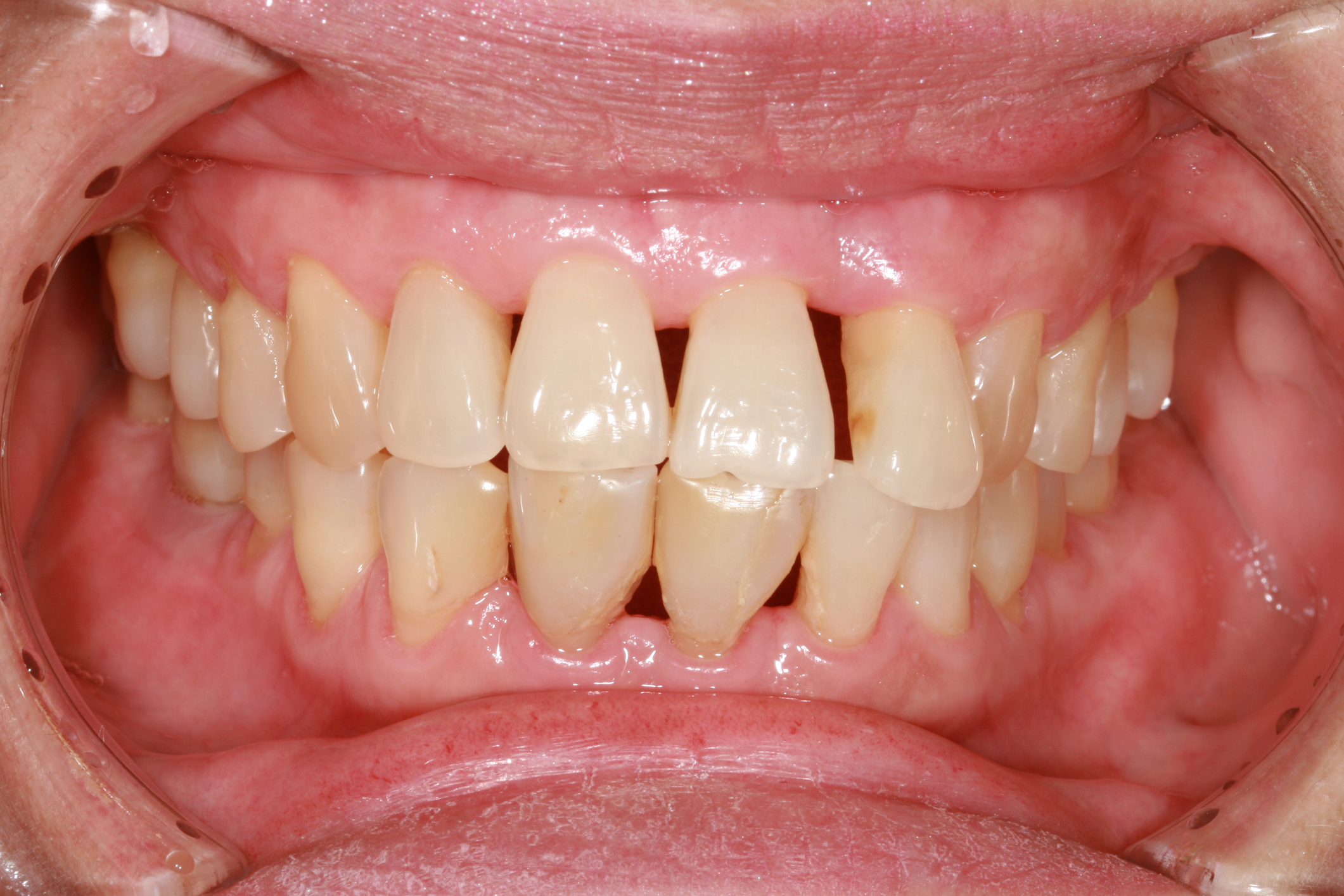
Gum recession.
How is your gum health? About half of all people over 30 suffer from periodontal disease, and this is the leading cause of gum recession. Gum recession is a problem, because when your gums recede too far, they can allow your teeth to fall out! Further, receding gums create pockets between the teeth and gums, and this can allow bacteria to grow and cause infections. In this way, even if your gum recession is not caused by periodontal disease, it can create an ideal environment for periodontal disease to progress. Once gums have receded, they don’t grow back, but there are some strategies you can employ to slow the recession. First, you need to know what is causing your gum line to recede.
- As mentioned, periodontal disease is a major cause of receding gums. The bacterial gum infections of periodontal disease can destroy not only gum tissue, but also the bone that holds the teeth in place. Catching periodontal disease in the early stage, called gingivitis, when the gums are simply inflamed, can help forestall its progression.
- It could be your genes. Sometimes, genetics just don’t work in your favor when it comes to your gums. About 30 percent of people have receding gums, leading to periodontal disease, no matter how well they care for their teeth.
- You might not be taking good care of your teeth. Poor oral hygiene can lead to tartar build-up, and when this happens, it can cause your gums to recede.
- On the other hand, you might be brushing too enthusiastically. Aggressive brushing can wear away your enamel and damage your gum tissue.
- Your teeth may be crooked. Believe it or not, misaligned teeth can wear on your gums. Teeth that don’t come together properly put too much force on the gums, causing them to recede.
- It might be hormones. Hormonal fluctuations, like the ones experienced during puberty, pregnancy, or menopause, can cause your gums to recede.
- Mouth trauma can damage your gums. If you get punched in the mouth or fall on your face, your teeth can be knocked loose, and your gums can sustain damage that causes recession.
- Your orthodontia may be the issue. It makes sense that using constant force to reposition your teeth could cause your gums to become inflamed and recede.
- If you grind your teeth, your gums might recede. In fact, receding gums may be your first warning sign that you grind your teeth at night.
- Tobacco use can lead to receding gums. Smoking and chewing tobacco are bad for your oral health in such a variety of ways that if you use tobacco, you really need to stop.
You might notice your gums receding, or you might notice some other warning signs. Your teeth may become sensitive to heat, cold, and sweets, or they may be sensitive when you’re brushing, flossing, or getting dental cleanings. You may also experience pain or discomfort near the gum line. Without treatment, gum recession could cause your teeth to feel loose. Fortunately, while receding gums won’t grow back, your dentist can help you slow the recession, as well as offering non-surgical and surgical treatments to improve the condition.
When you’re looking for a dentist to help with your teeth and gums, trust the dentist voted best in New York. At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Reasons Why your Teeth are Temperature Sensitive

Do you find that eating ice cream or drinking hot coffee causes pain in your teeth? You may have sensitive teeth. It’s a common condition, affecting about 45 million people in the United States, but it can be painful and difficult. What causes teeth to be temperature sensitive? More importantly, what can be done about it?
Your dentist can help you determine the underlying cause of the sensitivity, though the reason teeth become sensitive is typically always the same. Teeth are made of three layers, the enamel, the dentin, and the pulp. The enamel is the hard, outer layer of the teeth, and it protects the softer, inner layers. Below the enamel is the dentin, which is made up of microscopic tubes leading to the innermost layer- the pulp. Within that pulp is the nerve system of the teeth, and dental sensitivity happens when the dentin layers or the nerves are stimulated by something hot or cold. The cause of this stimulation varies.
Cold sensitivity can be caused by tooth decay or gum disease. It can also be the result of brushing too aggressively, using abrasive toothpaste, or using a hard-bristled toothbrush, which can all wear away at the enamel. Tooth grinding or clenching can chip the teeth or damage tooth enamel, which can also cause sensitivity to cold. Receding gums and cracks in a tooth can leave that tooth vulnerable to the cold. If your teeth are sensitive to heat, though, it could have a different cause. Dental treatments like teeth whitening can lead to heat sensitivity, and so can teeth cleanings, root planning, and dental crown or filling placement. If you consume a diet that’s high in acids, found in foods like coffee, tomato sauce, and wine, it can lead to enamel loss and heat sensitivity. People struggling with gum disease often have sensitive teeth, because 80 percent of tooth sensitivity begins at the gum line.
If your teeth are highly sensitive and react to both heat and cold, the best thing to do is see a dentist to determine the cause and the best course of treatment. If the sensitivity is minor, though, you may be able to manage it at home. You can reduce the discomfort of mild temperature sensitivity by making a few changes.
- Instead of letting hot and cold liquids touch your teeth, use a straw.
- Reduce your consumption of acidic foods.
- Change to a softer bristled brush and be careful not to brush too hard.
- Switch to a toothpaste for sensitive teeth.
- Ask your dentist which mouthwash to use; some mouthwashes can irritate your dentin and pulp layers.
- Wear a mouthguard to prevent teeth grinding at night.
There are also treatments that dentists offer to improve dental sensitivity. If you find that your sensitivity is not improving after a few days, talk to your dentist about the best treatment for you. It could be as simple as fluoride therapy, or it could be a more involved procedure like a root canal or a gum graft. Dental restorations like a filling, inlay, onlay or crown can also protect damaged teeth and help with sensitivity. Nervous about seeing the dentist? We provide sedation dentistry for your comfort.
If you are looking for a dentist to help with tooth sensitivity, it makes sense to choose the practice voted Best in New York. At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Simple Ways to Motivate You to Floss Every Day

Good oral hygiene is important for a healthy mouth, and one of the most effective ways to achieve it? That’s right—flossing! Flossing is one of the most important habits you can adopt to maintain good oral health. According to research, only 4 out of 10 adults floss daily and only 1 in 3 actually flosses correctly. Daily flossing helps prevent cavities, gum disease, and bad breath. But sometimes it’s hard to remember to do it every day. So here are some simple motivators that might help you get into the habit of regular flossing.
Find a Flossing Product That Works for You
The type of floss you use matters! Many people don’t realize that different types of floss work differently for different types of teeth and mouth needs. Waxed, non-waxed, disposable floss sticks, electric or water flossers—there are so many options available! If one type of product isn’t working well with your teeth and gums, try another! Experiment with different products until you find the perfect one for your personal oral hygiene routine.
Keep Your Floss in Sight
If you have your dental floss handy, you are more likely to remember to use it every day! Try keeping an extra package at the office or even in your pocket or purse wherever you go. You should also keep a container on the sink or bathroom countertop as a constant reminder that it’s time to floss every day!
Set A Goal
One of the best ways to make sure you stick with something is to set a goal. Make a goal that you can realistically achieve, like “I will floss at least twice a week for the next month.” Once you reach that goal, reward yourself by doing something special or purchasing something nice! This will help motivate you to keep going and eventually make daily flossing part of your routine.
Create A Chart
If setting goals isn’t quite your thing, another way to motivate yourself is by creating a chart or calendar that tracks your progress. Every day after you floss, mark it off in your chart or on your calendar as a reminder that you achieved your goal for the day. Seeing this progress can give you an added boost of motivation and encouragement!
Use A Reminder App
If neither of these methods seem like they’d work for you, consider downloading a reminder app onto your phone or laptop. With this type of app, all you have to do is set the time when you want it to remind you each day–it could be right before bedtime, so it becomes part of your nighttime routine–and then just follow through with the action when the reminder goes off!
Get Flossing!
Flossing every day is an important part of maintaining good oral hygiene and overall health. And while remembering to do it can be difficult at times, there are several easy strategies available that can help motivate and remind us so that we don’t forget! Whether it’s setting goals and rewarding yourself for reaching them, using visuals like charts and calendars, or using apps on our phones for reminders—these simple strategies can help ensure we stick with our daily flossing routine.
If any questions remain about flossing or other dental-related topics such as teeth whitening services offered at Park 56 Dental in New York City, please contact us today!
-
Understanding Your Gums
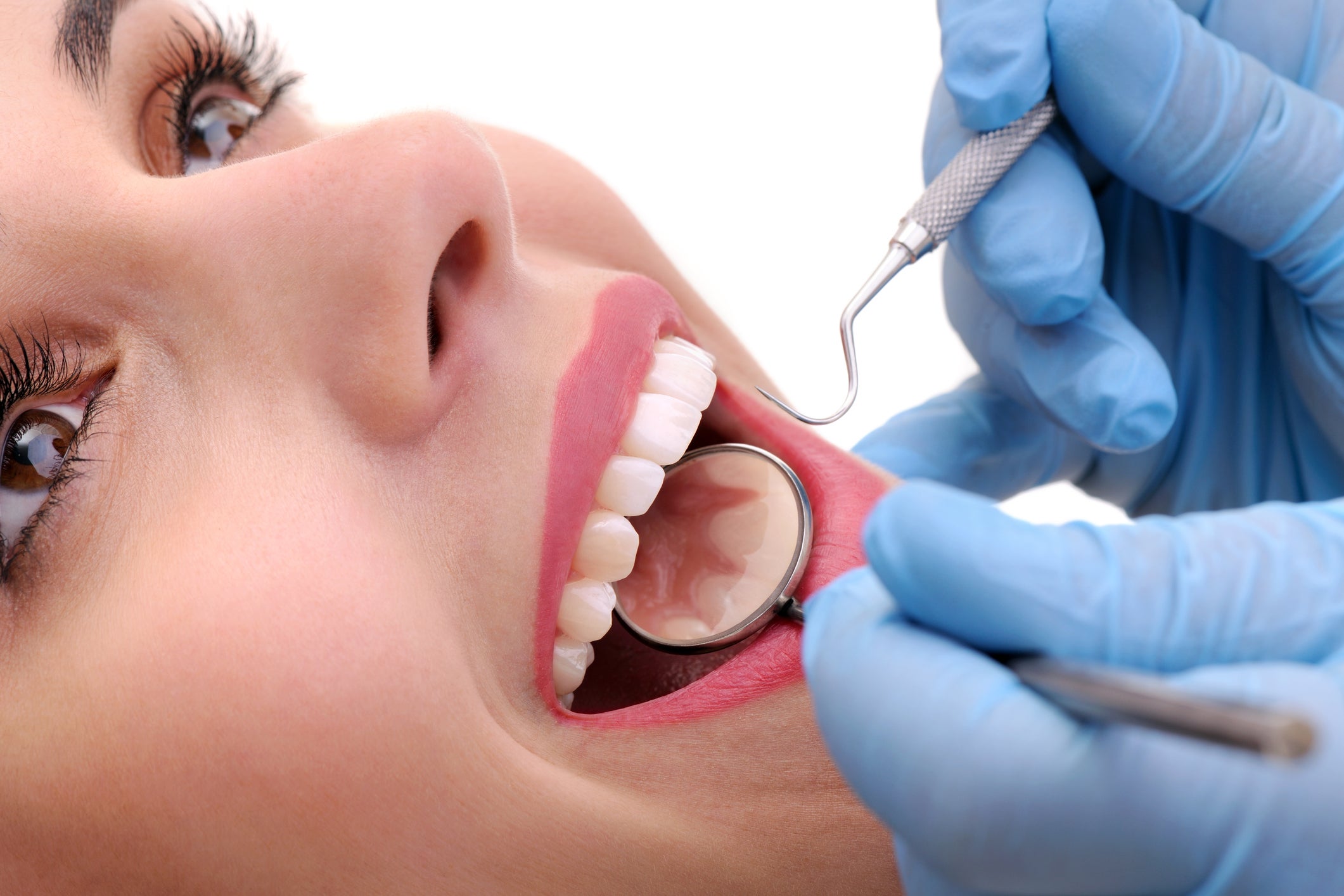
You know about cavities, and tooth decay, and how important it is to brush and keep your teeth healthy. But how much do you know about the health of your gums? The gums are an important part of your mouth, and if they’re not in good shape, your whole mouth can suffer. What do you need to know about your gums?
You might have noticed that your oral hygienist or dentist probes your gums during your regular check-ups. This is to determine if your gums are fitting snugly against your teeth. Unhealthy gums have pockets of space, and the deeper the pocket, the worse your gum health. It may feel like your gums are just being poked, but what the dentist is actually doing is measuring them. The tool used to probe gums is called a periodontal probe, and it’s essentially a tiny ruler. It is inserted into pockets in your gums, and the depth is recorded in millimeters.
Your dentist will keep track of these numbers as a preventive measure against periodontal disease (gum disease). Only your dentist can diagnose gum disease, but in general, 1 to 3 mm means the gums are generally healthy, 4 mm means you need to pay more attention to your oral care, 5 to 6 mm indicates gum disease, and anything over 6 means advanced gym disease. By regularly checking gum pocket depth, your dental team can catch periodontal disease early, when it’s still relatively easy to treat.
You can look for signs of gum disease at home, too. Swollen, sore, or bleeding gums could be a sign of gingivitis or periodontal disease. Gingivitis is the early stage of gum disease, and it happens when plaque builds up at the gumline. Once it progresses to periodontitis, it can affect the bone and tissue supporting your teeth. However, these symptoms can also be caused by other conditions and even vitamin deficiencies. Hormonal changes like pregnancy, illnesses like diabetes, infections, and vitamin C deficiency can all be responsible for gum problems, so you will want to see your dentist to get the right diagnosis.
What can you do to keep your gums healthy? First, pay attention to your oral care routine. Brush twice a day and floss once a day, brushing gently so that you don’t injure your gums. Consider using a water flosser, to clean below the gumline. Eat a nutritious diet, don’t use tobacco products, drink alcohol only in moderation, and take supplements, especially if you think you are not getting enough vitamin C. See your dentist for regular check-ups and cleanings, but in between visits, pay attention to your gums so that you can make a dental appointment if you notice signs of gum disease.
At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322
-
The Link Between Periodontal Disease and Premature Birth

It’s long been known that periodontal disease is a serious health problem. Beyond causing tooth loss and bleeding gums, periodontal disease can be detrimental to the whole body when bacteria from infected gums enters the bloodstream. Now, new research has revealed a link between periodontal disease and pre-term birth, showing that women with gum disease are substantially more likely to go into early labor than women with healthy gums.
The study, conducted by University Hospital Hradec Králové, Czech Republic, and led by Dr Vladimíra Radochová, from the department of dentistry, was published in the Journal of Clinical Periodontology. According to the Chief Executive of the Oral Health Foundation, Dr. Nigel Carter OBE, the research underscores the affect of oral health on a person’s overall health. The study showed that, of women who went into labor before 37 weeks of pregnancy, 45 percent had gum disease. By contrast, only 29 percent of women who experienced a perfect pregnancy had gum disease.
Worldwide, premature labor is the result of about 10 percent of all pregnancies. In the UK, the rate is about seven percent, and about 10 percent of babies in the United States arrive early, according to the Centers for Disease Control and Prevention. Premature birth can be the result of changes in the cervix or premature rupture of membranes, also known as “waters breaking.” So, what’s the link to periodontal disease?
It’s thought that bacteria in plaque traveling through the bloodstream to the placenta causes inflammation. Part of the problem is that it can be difficult for women to maintain good oral health while pregnant. Hormonal changes can make the gums more likely to be sore, swollen, and even bleed, because they’re more vulnerable to plaque. The women involved in the study who went into early labor were found to have eight times more plaque than the women with more favorable outcomes, and dental health that was four times lower. In addition to gum disease, women who had premature labor were more likely to have untreated tooth decay or fillings.
The takeaway from the study is that it’s important for a woman to care for her mouth to help ensure a healthy pregnancy. Brushing twice a day and flossing can help maintain oral health, and refraining from smoking and alcohol consumption can also reduce the chance of gum disease. Most important are regular dental appointments, to stay on top of oral health issues and keep periodontal disease at bay.
During pregnancy and every other stage of life, when you’re looking for excellent dental care and advice you can trust, choose the practice that was voted best dentist in NYC! At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
The Link Between Your Oral Health and Alzheimer’s

It seems far-fetched to say that your oral health and Alzheimer’s disease could possibly be connected. However, this is exactly the claim that research is beginning to suggest.
As research has been done to compare the brains of people with and without Alzheimer’s disease, scientists have discovered that individuals who suffer from Alzheimer’s disease have an increase in levels of certain bacteria that are also responsible for the cause of gum disease, such as porphyromonas gingivalis and a toxic enzyme that it creates called gingipains. Gingipains is secreted from this bacteria and has been found to destroy the brain’s neurons. This similarity between gum disease and Alzheimer’s is enough to suggest that the prevention of gum disease may also be connected to the possible prevention of Alzheimer’s
In a different study led by the CDC’s National Center for Health Statistics, baselines were taken and individuals were tracked with follow-up data kept for up to 26 years. Up to 19 antibodies were found that are associated with Alzheimer’s with the most fatal being, again, porphyromonas gingivalis and its production of the toxic enzyme gingipains.
So, it makes sense to work hard to prevent gum disease and, therefore, reduce the risk of MANY other problems!!
What do I do if I already have gum disease?
Healthy oral hygiene habits can decrease the risk of gum disease. Continue to improve and maintain healthy habits, including:
- flossing daily
- brushing your teeth 2-3 times a day
- using antibacterial mouthwash
- changing your toothbrush every 3 months
- being intentional about what foods and drinks you comsume
Remember, also, to visit your dentist at least 2 times a year for cleanings. If your teeth are showing signs of plaque build-up, there is a procedure for deeper cleaning of the teeth and gums that may be right for you. Continuing to care for your teeth is of the utmost importance. Your health and wellbeing are so valuable, especially to those whom you love!
How can I protect myself?
Keep learning and researching! Education is the key to making informed and improved decisions. Some of your health journey is genetic, but some is left up to you and the choices that you make for taking care of yourself. You may not be able to change past decisions but you can certainly work toward staying the healthiest you can possibly be. Whether you have always been on top of your oral health and hygiene or you have room for improvement, remember that your teeth and gums impact your whole body’s wellness.
While this research is still undergo, you have the ability to be proactive. Clean teeth make for a healthier you! Stay informed and maintain that amazing smile! Schedule a cleaning today so that you can maintain healthy teeth, heart, and mind!
You are worth the time, energy, and expense of a happy, healthy smile! So, go ahead and take some much needed time to invest in yourself and your future! You’ll be so very glad that you did!!! Call Park 56 Dental today at
-
Why Your Gums Hurt When Brushing Your Teeth
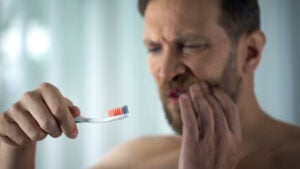
Do your gums hurt when you brush and floss? Is there blood in your toothpaste when you spit into the sink? This usually means one of two things—either you’re being too rough when you brush and floss, or you’re developing gum disease. To rule out other more serious problems, be sure to visit your dentist. Otherwise, explore these solutions to help prevent your gums from hurting when you brush your teeth.
When Your Gums Hurt Because of Rough Brushing and Flossing
It’s easy to brush too hard when you’re trying to be thorough. However, you can easily irritate your sensitive gum tissue if you scrub aggressively. Here’s how to clean your teeth while protecting your gums:
- Use a soft-bristled toothbrush.
- Brush in gentle, circular motions.
- Consider switching to an electric toothbrush.
- When flossing, follow the curve of your teeth and avoid snapping the floss against your gums or using a sawing motion.
When Your Gums Hurt Because of Gum Disease
Mild gum disease, known as gingivitis, starts when a sticky film of bacteria called plaque builds up along the gum line. Ignoring gingivitis can lead to periodontal disease and, eventually, severe periodontitis. If your gums are swollen, red, irritated, and hurt when you brush, talk to your dentist about starting treatment.
Other Reasons Why Your Gums Hurt
There are many other potential causes of painful gums, including:
- Canker sores
- Tooth abscesses
- Tobacco use, including cigarettes, vaporizers, and chewing tobacco
- Hormonal changes during puberty, menstrual cycles, pregnancy, and menopause
- Thrush, a type of yeast infection
- Ill-fitting oral devices, including braces, retainers, dentures, and mouthguards
- Chemotherapy drugs
How to Sooth Sore Gums
In addition to brushing and flossing more gently, treating gum disease, and tackling other causes of painful gums at the source, try these tips to soothe your sore gums:
- Rinse your mouth with warm saltwater.
- Rinse with mouthwash containing hydrogen peroxide.
- Take over-the-counter pain relievers.
- Apply numbing gel to the tender area.
- Avoid spicy or acidic foods to avoid further irritation.
- Eat yogurt with live cultures to balance the bacteria in your mouth.
Discuss Your Symptoms with Your Dentist
If your gums hurt or bleed for over a week, and your attempts to treat the problem at home aren’t working, it’s time to contact your dentist. A professional teeth cleaning can remove the stubborn plaque irritating your gums. Your oral hygienist may also perform a deep-clean called root planing and scaling if you have gum disease.
Don’t ignore painful gums—stop by Park 56 Dental in NYC to discuss your symptoms with our dentist. We can examine your gums and teeth and recommend the proper treatment. Our office has been voted the best dentist in New York, with over 20 years of experience serving the 10022 zip code area, so you can trust us to take great care of your smile! Call us at (212) 826-2322 to set an appointment today.
-
How to Prevent Gum Recession

Receding gums are a common oral health problem. You know your gums are receding if you have less gum tissue than you used to and your teeth look longer than normal. What you’re seeing is the exposed tooth root, which may be sensitive to hot and cold temperatures. Gum tissue doesn’t grow back, so it’s important to prevent gum recession before it’s too late.
- Brush your teeth gently: It’s a misconception that the more aggressively you brush, the cleaner your teeth become. Not only does vigorous brushing wear down tooth enamel, but it also irritates your gums. Switch to a soft-bristled toothbrush, and be careful about how much pressure you use when brushing each morning and night.
- Floss daily: Flossing targets the hard-to-reach places between your teeth and along the gum line. Scraping away plaque and stubborn food particles from these areas is critical to keep your gums healthy and prevent them from receding.
- Stop smoking: Tobacco use of any kind is horrible for your oral health. It leaves a sticky film in your mouth that can cause gum recession if not removed thoroughly. Stop smoking to promote gum health, prevent tooth stains, and reduce the risk of oral cancer.
- Eat a nutritious diet: Gum tissue, like the rest of your body, needs adequate vitamins and minerals for optimum health. Some of the best foods for a healthy smile include apples, carrots, leafy greens, plain yogurt, and almonds.
- Wear a mouthguard: Do you grind your teeth at night? If you’re not sure, your dentist can diagnose this condition, known as bruxism. Then, you can look into getting a custom mouthguard to protect your teeth and gums while you sleep.
- Straighten your smile: Crooked teeth and a misaligned bite place excess pressure on your jawbone and gums, making gum recession more likely. Invisalign is the invisible way to straighten your teeth and keep your gums healthy.
- Avoid mouth piercings: Lip and tongue rings are a surefire way to irritate your gums and cause them to recede. So play it safe and stick to ear piercings to keep your mouth free of foreign objects.
- Visit the dentist: The American Dental Association recommends that most people visit the dentist every six months for a checkup and cleaning. During your exam, a hygienist will remove tartar and plaque from your teeth that can irritate the gums. Your dentist will also check for signs of recession and offer personalized tips to prevent the problem from getting any worse.
If you notice receding gums or other signs of gum disease, reach out to Park 56 Dental. We’ve been voted the best dentist in NYC, so you can rest assured that our team will take great care of you. We offer effective treatments to help slow or even reverse gum disease and recession, including root planing and scaling, flap surgery, and bone and tissue grafts. To learn more, please call us at (212) 826-2322 or contact us online today.
-
Being Voted NYC’s Best Dentist

If you’re looking for the best dentist in NYC, look no further than Park 56 Dental Group. We’ve been voted NYC’s best dentist, and it’s no wonder. We provide personalized, quality dental care to a clientele that appreciates our comfortable, spa-like environment.
Our status as the best dentist is confirmed by our many five-star reviews. Clients say we’re “very thoughtful, caring and all around well organized”, “kind and wonderful”, “compassionate and professional”, and that our practice “makes going to the dentist a pleasure”. One customer characterized our staff by saying the “entire office was informative, compassionate and worked together like a team.” What makes us the best dentist in NYC? We think it’s a combination of several factors.
- Comprehensive Services: We provide routine dental services and so much more! Taking care of your teeth is an important part of caring for your overall health, so visiting the dentist regularly is vital. We provide oral cancer screenings for your peace of mind, and our cleanings and oral exams can save you from dental care problems and a wide range of health issues. We also offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency and sedation dentistry
- Expert Cosmetic Dentistry: Our restorative dentistry will improve your smile and boost your confidence. The services we provide include teeth whitening, contouring/tooth reshaping, bonding, bridges, veneers, dental implants, tooth colored fillings, and smile makeovers.
- Quality Care in a Comfortable Facility: We’re committed to providing your entire family with safe, gentle, high-quality dental care. We’re sensitive to your needs and want you to be comfortable while we provide you with the best care possible. Feel free to stop by our office and take a tour of our facilities.
- Patient-centered Practice: Our knowledgeable, compassionate dentists and staff excel at providing personalized care, and we’ll work together to meet your individual needs. We’ll answer any questions you may have, providing expert advice, and we’ll help if you struggle with dental anxiety. We want you to feel comfortable, safe, and relaxed at our office, and we even offer sedation dentistry for patients who request it. You can meet our team, take a walk through our office and treatment areas, and learn more about the treatments we provide.
If you want to trust your dental care to the very best dentist in NYC, call Park 56 Dental Group. We offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
RECENT POSTS
categories
- Uncategorized
- Cosmetic Dentistry
- Veneers
- Healthier Teeth
- Teeth Whitening
- Dental Health
- Video
- Dental Emergencies
- Invisalign
- Dental Implants
- Root Canal
- Sedation Dentistry
- Infographic
- Dental Crowns and Bridges
- Dental Anxiety
- Gum Disease
- COVID-19
- Bad Breath
- New York Dentist
- Cut out sugar
- General Dentistry
- Oral Health
- Oral Cancer
- Dry Mouth
- Gum Health
- Toothache
- Dental Sealants
- Cavities
