-
Preventing Dental Emergencies: Tips and Tricks to Keep Your Teeth Safe

Man taking care of teeth to prevent dental emergencies.
Dental Emergencies Are a Problem
When you have a dental emergency, it’s more than just inconvenient, it’s also traumatic. Painful and stressful, accidents can lead to hours at the emergency dentist and, in some cases, permanent tooth loss or severe gum bleeding. While there’s no way to prevent accidents completely, there are a few steps you can take to avoid most dental emergencies.
Your Dentist is Your Ally
Regular dental visits can help keep your teeth healthy and strong, catching problems before they become emergencies. What’s more, your dentist can recommend measures like sealants to protect your teeth from decay or an oral appliance to guard against bruxism. See your dentist twice a year for preventive care and a cleaning. Being proactive about preventive dental care can be much less costly and stressful in the long run.
Tips for Keeping Your Teeth Safe
- Practice good dental hygiene. At home, brush twice a day, floss at least once, and use mouthwash. Keeping your teeth clean can help prevent cavities, gum disease, cracks, fractures, and infections. Having your teeth deep cleaned at the dentist’s office twice a year gives added protection.
- Eat a tooth-strengthening diet. Eat a nutrient-dense diet, taking care to eat foods like leafy greens, fresh fruits and vegetables, and calcium-rich foods. Limit consumption of processed foods and sugary sweets, which can cause plaque buildup and feed the bacteria that cause tooth decay.
- Protect your teeth during sports. If you participate in sports, talk to your dentist about getting a custom-made mouthguard. This can make a big difference in keeping your teeth from being knocked out or damaged. You might also want a mouthguard to wear at night, to prevent teeth grinding.
- Manage your stress. Stress is bad for your whole body, and it can damage your teeth. People who are stressed may absentmindedly chew on hard things, and stress can cause people to grind their teeth. Embrace techniques like mindfulness, practice yoga, or find other healthy ways to manage your stress.
- Remember that teeth are not tools. We’ve all used our teeth for something we shouldn’t from time to time, when we can’t find the scissors, or the bottle opener is in another room. It could be fine, but then on the other hand, it only takes once for a tooth to crack. The convenience of not having to rummage through a drawer or ask for help is not worth risking your teeth.
- Don’t hesitate to seek dental care. Don’t let a dental emergency get out of hand. If you have a toothache, seek treatment as quickly as possible. Pain is an indication that something is not right, and getting treatment quickly can mean the difference between a routine procedure and serious oral surgery.
Park 56 is Here for Your Emergencies
If you’re looking for a dentist in New York, why not choose the dentist voted best in the city? At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Emergency Dental Care

Woman Suffering From Dental Emergency
It’s natural to feel alarmed when you experience a toothache or get hit in the mouth. Is the pain a minor annoyance, or are you about to face a dental emergency? Understanding the difference between urgent and non-urgent dental scenarios helps you act quickly when necessary to maintain your radiant smile.
Deciding If it’s a Dental Emergency
Dental emergencies come in many forms. Some issues require immediate attention to alleviate pain and improve the chances of saving a damaged tooth. Watch for these symptoms of a dental emergency:
- Intense toothache
- Excessive bleeding
- Trauma to the face
- Loose or knocked-out tooth
- Broken or chipped tooth with a large chunk missing
Other issues aren’t a major cause for concern and can wait for a regular appointment. Examples of non-urgent situations include:
- Lost filling or crown
- Cracked tooth without pain or sharp fragments
- Mild toothache with no other symptoms
The Crucial First Response
If you determine you’re having a dental emergency, knowing how to respond is crucial. Follow these tips until you can get to an emergency dentist:
- Treating a toothache: Rinse your mouth with warm water and gently floss to remove trapped food. If the pain persists, take over-the-counter pain relievers. Then, book a dentist appointment to find out what’s wrong.
- Treating excessive bleeding: Rinse with a saltwater solution. Then, apply a clean, damp piece of gauze or a cool, used tea bag to the area. If bleeding continues after 15 to 20 minutes, seek medical help.
- Treating a loose tooth: A loose tooth in adults is not normal. Avoid wiggling it to prevent further damage, and contact your dentist for a professional evaluation.
- Treating a knocked-out tooth: Handle the tooth carefully. Avoid touching the root, rinse it with water if dirty, and try reinserting it into its socket. If that’s not possible, store the tooth in a container of milk or use a tooth preservation kit and go to the dentist immediately.
- Treating a broken, cracked, or chipped tooth: Rinse your mouth with warm water and apply a cold compress. Over-the-counter pain relievers minimize discomfort. Contact your dentist right away, even if there’s no pain, because the tooth may be damaged internally.
The Role of an Emergency Dentist
An emergency dentist handles urgent cases with the proper tools and training. From antibiotics for infections to quick dental procedures for saving a knocked-out tooth, these professionals provide immediate relief and ensure long-term oral health.
Park 56 Dental is your go-to provider for same-day emergency dental care. We have served patients in the 10022 zip code and surrounding areas since 1997. We even boast the title of NYC’s best dentist. Our office feels more like a spa, and we focus on giving personalized, quality dental care to each patient. Our team has experience with everything from general dentistry and sedation dentistry to oral surgery and endodontics.
The next time a dental emergency strikes, you can count on us! Call Park 56 Dental at (212) 826-2322, and we’ll help you get your oral health back on track.
-
How to Avoid Dental Abscesses

Dental abscesses are one of the most painful conditions that can affect your teeth and gums. If you think you may have a dental abscess, it’s important to see a dentist right away so that the infection can be treated and the pain relieved. Read on to learn more about dental abscesses and what to do.
What Are Dental Abscesses?
A dental abscess is an infection that can occur around the teeth and gums. This infection is often the result of bacteria that enters the mouth through a tooth or gum injury. The bacteria then multiply and cause an abscess, which is a pus-filled pocket that forms at the site of the infection.
Dental abscesses can be extremely painful and may require treatment by a dentist or other medical professional. If left untreated, dental abscesses can lead to serious health complications such as sepsis (a potentially life-threatening condition caused by infection).
What Are the Symptoms of Dental Abscesses?
The symptoms of dental abscesses can vary depending on where the infection is located. The most common symptom of a dental abscess is severe pain. This pain is often described as throbbing or pulsating and may be worse when lying down or when pressure is applied to the affected tooth. Other symptoms of a dental abscess include:
- Swelling in the face, jaw, or neck
- Redness in the mouth or on the skin around the mouth
- Sensitivity to hot or cold temperatures
- Bad breath
- Fever
How Are Dental Abscesses Diagnosed?
If you think you might have a dental abscess, it is important to see a dentist right away. Your dentist will ask about your symptoms and medical history. They will then examine your mouth, teeth, and gums. X-rays may be taken to confirm the diagnosis.
How Are Dental Abscesses Caused?
Dental abscesses are usually caused by bacteria that enters the tooth through a crack or cavity. Once the bacteria gets inside, it can start to multiply and cause an infection.
What Are the Risks of Abscesses?
If left untreated, dental abscesses can lead to more serious health problems such as: sepsis (a blood infection), meningitis (an infection of the brain and spinal cord), and even death.
How Can I Prevent Dental Abscesses?
Dental abscesses can be painful and dangerous, so it’s important to take steps to avoid them. Park 56 Dental in New York City offers the following tips:
- Brush and floss regularly. This helps remove plaque and bacteria from your teeth and gums, which can lead to an infection.
- See your dentist regularly for checkups and cleanings. This allows your dentist to spot any problems early and take steps to prevent an infection.
- If you have a toothache, don’t wait to see a dentist. This could be a sign of an infection.
- If you have an injury to your mouth, see a dentist right away. An injury can lead to an infection if not treated properly.
- Eat a healthy diet. This helps keep your immune system strong, which can help fight off infection.
How Can Park 56 Dental in NYC Help Treat my Dental Abscess?
The treatment for a dental abscess will depend on the severity of the infection. In some cases, the abscess may need to be drained by a dentist or other medical professional. The pus that is drained from the abscess will usually contain bacteria, so it is important that the area is cleaned thoroughly to prevent the infection from spreading. In some cases, antibiotics may be prescribed to help clear the infection. In some cases, they may also need to perform a root canal procedure to remove the infected tooth. If the abscess is large or does not respond to treatment, surgery may be necessary.
If you think you may have a dental abscess, don’t wait to get it treated. Call Park 56 Dental today at (646) 679-3989 to schedule an appointment.
-
Dental Emergency: What to Do When a Tooth Gets Knocked Out

Did you know that more than five million teeth are knocked out every year in children and adults? If this happens to one of your loved ones, don’t worry! Quick action can improve your odds of saving the tooth.
Causes of Knocked Out Teeth
Teeth get knocked out for various reasons that all involve an impact to the face. Most often, a tooth becomes knocked out during a contact sport when the participant failed to wear a mouthguard. The most common ways that teeth get knocked out include:
- Sports injuries
- Car accidents
- A fight
- Tripping or falling
Sports-related oral trauma ranges from a chipped tooth to having a tooth completely knocked out. By taking quick action, caretakers can make a big difference on salvaging the damage.
Preserving a Knocked-Out Tooth
Many are unaware that a tooth can be saved even if it is knocked out. Learn what to do immediately after a tooth is knocked out so you can restore your prior smile’s beauty. The following steps are recommended by the American Association of Endodontists to save a tooth that has been knocked out:
- Delicately pick up the lost tooth by the crown (also known as the chewing surface.)
- Use water to rinse the tooth. Only water, nothing else.
- Gently replace the tooth in the original socket at once. Keep it in place with your fingers or by biting down softly.
- Keep the tooth moist in your mouth. If it won’t stay in the socket, place in next to your cheek in your mouth, or in a small container of milk.
- Visit your dentist, endodontist, or emergency department within 30 minutes of the accident. (Some teeth can still be saved if it has been outside the mouth for more than hour but contact your dental provider for specific instructions.)
In the dentist’s office or emergency department, the tooth will either be re-implanted or splinted to the nearby teeth for a period of two-eight weeks. A root canal procedure will be needed for long-term survival of the tooth.
Other Reasons a Tooth May Fall Out
If you lose a tooth due to periodontal disease, the steps listed above will not save the tooth. Prevent this type of tooth loss by proactively visiting your dentist every six months and performing the proper oral care steps at home.
Park 56 Dental offers same-day emergency appointments to get you the critical care you need when a tooth is knocked out. We understand that dental injuries require immediate, personalized care to put your mind at ease and to restore your smile.
Contact us today at (646) 679-3989 if you have any questions about a dental emergency or what to do. Your safety and well-being are our first priority!
-
How to Find the Perfect Dentist

When you’re looking for a dentist, the number of options available can be overwhelming. Factor in anxiety about going to the dentist, and it’s easy to see how finding a dentist could seem like a daunting task. Don’t worry! We’ve got some tips to help you find the perfect dentist for you and your family.
- Ask people you trust. Word of mouth can be the most effective way to find the right dentist. Make a list of dentists recommended to you by family members, close friends, co-workers, and your primary care physician. Don’t worry too much about whether the dentists are in your network; you can often maximize your insurance benefits out of network. Armed with your list, you can begin to narrow the search.
- Find a full-service dentist. Don’t choose a dental practice with limited specializations. Rather, look for one who performs a wide range of services, all in one practice. You don’t want to have to go through the process again when you need a different kind of dental work.
- Check the dentist’s credentials. Make sure your dentist is board certified and has a current state license as well as a clean disciplinary history. Healthgrades.com and your state website will have information about your dentist’s medical school, training hospital, certifications, and malpractice and disciplinary history. Look for solid credentials and plenty of experience.
- Read online reviews but don’t put too much stock in them. Patient reviews can give some insight into how the dental practice is operated. On the other hand, online reviews can be manipulated. Read them, taking note of what patients have to say, but pay special attention to the dentist’s responses to the reviews. If the dental practice responds in a positive way to online reviews, regardless of whether the review is positive or negative, it indicates that the dentists in the practice care about their patient.
- Tour the office. While you’re there, ask questions about things like office hours, technology, the dentists’ training, continuing education, their approach to preventive dentistry, emergency appointments, and financing. Note the cleanliness of the office, friendliness of the staff, and willingness to answer questions.
- Think about your personal preferences. Do you prefer a dentist of a certain gender? Are telehealth appointments important to you? Which dental services do you believe you’ll need most often? Is flexible scheduling a priority for you? When you meet a dentist who checks all the boxes and makes you feel comfortable, that’s probably the perfect dentist for you!
If you’re looking for the perfect dentist, choose the practice that was voted best dentist in NYC! At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Being Voted NYC’s Best Dentist

If you’re looking for the best dentist in NYC, look no further than Park 56 Dental Group. We’ve been voted NYC’s best dentist, and it’s no wonder. We provide personalized, quality dental care to a clientele that appreciates our comfortable, spa-like environment.
Our status as the best dentist is confirmed by our many five-star reviews. Clients say we’re “very thoughtful, caring and all around well organized”, “kind and wonderful”, “compassionate and professional”, and that our practice “makes going to the dentist a pleasure”. One customer characterized our staff by saying the “entire office was informative, compassionate and worked together like a team.” What makes us the best dentist in NYC? We think it’s a combination of several factors.
- Comprehensive Services: We provide routine dental services and so much more! Taking care of your teeth is an important part of caring for your overall health, so visiting the dentist regularly is vital. We provide oral cancer screenings for your peace of mind, and our cleanings and oral exams can save you from dental care problems and a wide range of health issues. We also offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency and sedation dentistry
- Expert Cosmetic Dentistry: Our restorative dentistry will improve your smile and boost your confidence. The services we provide include teeth whitening, contouring/tooth reshaping, bonding, bridges, veneers, dental implants, tooth colored fillings, and smile makeovers.
- Quality Care in a Comfortable Facility: We’re committed to providing your entire family with safe, gentle, high-quality dental care. We’re sensitive to your needs and want you to be comfortable while we provide you with the best care possible. Feel free to stop by our office and take a tour of our facilities.
- Patient-centered Practice: Our knowledgeable, compassionate dentists and staff excel at providing personalized care, and we’ll work together to meet your individual needs. We’ll answer any questions you may have, providing expert advice, and we’ll help if you struggle with dental anxiety. We want you to feel comfortable, safe, and relaxed at our office, and we even offer sedation dentistry for patients who request it. You can meet our team, take a walk through our office and treatment areas, and learn more about the treatments we provide.
If you want to trust your dental care to the very best dentist in NYC, call Park 56 Dental Group. We offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
How Often Should You Be Going to the Dentist?

How often do you see your dentist? About one hundred million Americans skip out on regular dental checkups, even though seeing a dentist regularly is vital for good oral health. Your dentist probably encourages you to come twice a year, but is that really necessary?
Truthfully, there’s little research supporting the twice a year recommendation. So, how often should you be going to the dentist? It depends on a few factors. Some people need to go to the dentist more than twice a year. This high-risk group includes pregnant women, smokers, people prone to plaque build-up or cavities, those who have gum disease or diabetes, and anyone with a weak immune response. People who practice excellent oral hygiene and show no signs of gum disease or cavities may be able to get away with going to the dentist less often than twice a year, but that is something to discuss with the dentist.
Even if you’re diligent about brushing twice a day and flossing daily, seeing your dentist regularly is important. That’s because dentists and dental hygienists can spot problems you can’t see and prevent them from becoming major issues. When you go to the dentist, here’s what you can expect:
- X-rays: At the beginning of your appointment, the dental hygienist will take any x-rays you need so that the dentist can look at them while your teeth are being cleaned.
- Cleaning and Polishing: Using scalers and other dental tools, the hygienist will gently remove plaque and tartar from tooth surfaces and just below the gum line. Your teeth will then be polished with a paste, and the hygienist will floss between your teeth. During the cleaning, the hygienist will let you know if there are any areas to which you need to pay more attention when brushing and flossing, and instruct you on proper brushing and flossing techniques.
- Oral cancer screening: By examining your palate, tongue, throat, inside of cheeks, and other parts of your oral cavity and feeling the outside of your jaw and throat, your dentist will be able to spot any signs of cancer. Because oral cancer is most successfully treated when detected early, this screening is very important.
- Cavity detection: The dentist will examine your teeth for cracks, chips, decay or other damage, and the hygienist will chart any teeth that require treatment.
- Gum assessment: Your dentist will check for signs of gingivitis or periodontal disease. Gum disease is reversible when detected in the early stages.
- Dental appliance check: Because dental appliances don’t last forever, the dentist will check to see if anything needs replacing.
At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Should You Visit the Dentist During the Coronavirus Pandemic?
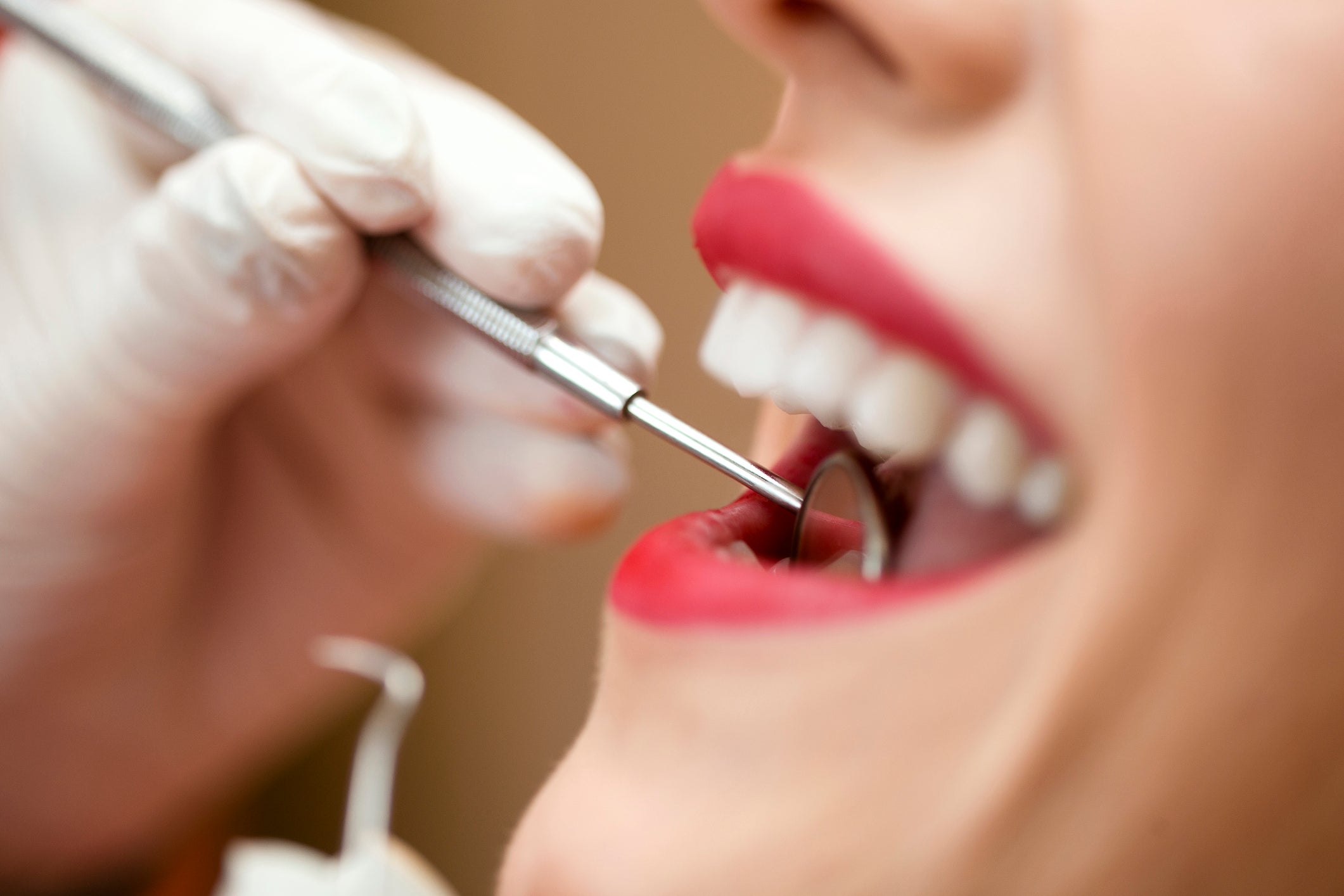
For several weeks in early 2020, dentists in New York City and elsewhere across the globe were required to stop providing non-urgent care in response to the novel coronavirus pandemic. As we resume our “new normal,” many patients are asking—is it still too early to visit the dentist?
Rest assured that the American Dental Association (ADA) and the Centers for Disease Control and Prevention (CDC) are now allowing patients to return to the dentist for routine cleanings, cosmetic dentistry, and other elective services—with a few changes in place. Here’s what you should know before visiting the dentist during the COVID-19 pandemic.
Is My Dentist’s Office Safe?
Germs are everywhere, but healthcare facilities, including dentist’s offices, have always been among the cleanest places you could go. Many safety guidelines have been the norm for years, including regularly washing your hands, sterilizing tools, and discarding certain gear and needles after a single use.
In light of the pandemic, many dentists, including Park 56 Dental in NYC, are doing even more. Here are some of the steps we’re taking to ensure patient safety and comfort:
- Conducting pre-visit health screenings and contactless temperature checks for all visitors and staff
- Making masks and hand sanitizer available upon request
- Staggering check-ins to minimize wait times and help maintain social distancing
- Holding virtual appointments to answer questions or conduct follow-ups
How “Essential” are Dentist Visits?
The fact that dentist offices were shut down for everything but emergency procedures could make some people think that routine teeth cleanings aren’t that important. However, the condition of your teeth and gums can greatly impact your overall health. In fact, putting off routine cleanings could compound dental problems and other health issues in the months and years to come.
The practical precautions that dentist offices are currently taking are effective at reducing the risk of coronavirus transmission while allowing you to care for your teeth and gums. Skipping your appointments any longer than necessary is simply not worth the risk to your oral health.
What to Consider Before Going to the Dentist
Social distancing is the best way to slow the spread of the coronavirus. If you have symptoms of COVID-19, you should self-isolate for 14 days. In short, cancel your dentist appointment if you’re not feeling well. You’ll be sent home if you come in with a cough, fever, or shortness of breath. You should also stay home if you think you have been around anyone who has the coronavirus, whether or not they have tested positive.
Park 56 Dental in NYC is open for business! Anything that can be done remotely, such as payments or health questionnaires, will be handled over the phone or via email. We are taking COVID-19 restrictions seriously and place your safety above all else. Please call us at (212) 826-2322 or contact us online to ask questions about our coronavirus precautions or to schedule an appointment. We look forward to hearing from you soon.
-
What is a Dead Tooth?

You may not think of your teeth as being alive, but they are. The outer shell, called the enamel, is the hardest substance in the human body. However, the nerves and blood vessels at the heart of your teeth are soft and vulnerable. If this inner layer (known as the pulp) becomes damaged, blood may stop flowing. A tooth with no blood flow is called a “dead” tooth. Without treatment, this tooth may become infected or abscessed and will eventually fall out.
What Causes a Dead Tooth?
Trauma or injury is a common reason for a tooth to die. Falling or being hit in the mouth can cut off the blood supply to a tooth or even cause blood vessels to burst. With no blood flow, the nerve inside the pulp dies.
Tooth decay is another possible cause. Without consistent dental hygiene habits, cavities can start to form. Left untreated, decay slowly eats through the tooth toward the sensitive pulp, eventually causing an infection. Inflammation may cut off blood flow to the pulp, causing the tooth to die.
How to Spot a Dead Tooth
It isn’t always easy to identify a dead tooth. Only a dental professional can pinpoint signs of restricted blood flow and a dying tooth in its early stages, which is why regular dentist visits are so important. Before long, though, the problem will soon become apparent.
Pain is the first symptom to watch out for. This may seem odd because the nerve inside your tooth is dead, but that’s not where the pain comes from. Bacteria and dead nerve remnants touching the extremely sensitive nerve endings around your tooth, called the periodontal membrane, are the source of your pain.
A change in color comes next. Dead teeth often darken over time as red blood cells die. This is very similar to developing a bruise. If a single tooth in your mouth gradually becomes yellow, gray, or black, visit the dentist right away.
Signs of infection could also appear if the dead tooth doesn’t receive treatment. You may notice swelling, a bad taste in your mouth, or an inflamed sore on your gums.
Treatment for a Dead Tooth
A root canal is the first option. Dentists want to avoid removing teeth whenever possible, and this procedure could save a dead or dying tooth. It involves removing all signs of decay and infection from deep within the tooth. Then, the dentist fills and seals it. In many cases, a crown is needed following a root canal.
Tooth extraction is the next choice. Even if your dentist can’t save your tooth, prompt treatment is necessary to avoid other complications. Once removed, you have several options for replacing the missing tooth, including an implant, bridge, or partial denture.
Park 56 Dental offers tooth care and smile restorations out of our spa-like, patient-centered New York dentist office. If you notice signs of a dead tooth, please contact us online or call us at (212) 826-2322 to schedule an appointment.
-
The Importance of Having your Cavities Filled

Even if you brush and floss religiously, doing your best to have pristine teeth and perfect oral health, you’re likely to one day have a cavity. If this happens, don’t delay treatment. It’s important to get any cavities filled as soon as possible, for many reasons.
- Tooth decay, left to its own devices, will spread. If you ignore a cavity, the decay will soon spread to the area around the cavity. Then you’ll not only have a bigger cavity than you originally had, but you may also have additional cavities as well. Getting it filled will solve the problem and keep the damage from spreading.
- Bacteria from a cavity is unlikely to stay in your mouth. An unhealthy tooth won’t just affect nearby teeth: it will spread bacteria as far as it can. Bacteria in your mouth is not ideal, but once it gets into your bloodstream and makes its way to other parts of the body, it can be extremely dangerous.
- Fillings keep your smile intact. If you don’t get a cavity filled in a timely manner, you may end up having to have the tooth removed entirely. Dental implants can solve the problem of missing teeth, but they’re much more expensive than fillings and require a much more complicated process. You’ll have a hole in your smile until you can get the implant, and this can compromise the bone in your jaw.
Those are pretty compelling reasons to get your cavities filled, but did you know there are different types of fillings? Each material used in fillings has its pros and cons, and your dentist will be able to help you determine which is right for you.
- Amalgam fillings have been around for over a century. They’re strong and ideal for cavities in the molars, because they can take the impact of chewing. Made of a combination of several metallic elements, they are sometimes visible when you laugh or smile, but they’re some of the least expensive cavity-filling materials.
- The other most common filling material is composite fillings. Sometimes called composite or filled resins, they’re made of a combination of glass or quartz filler. They can be made to match the color of your tooth, and they’re good in areas involved in moderate chewing.
- Metals, ceramic, and glass ionomer are also used as fillings. Gold and silver are often used, and these metallic fillings can last 10-15 years. Ceramic or porcelain fillings are attractive but expensive, and glass ionomer fillings can release fluoride to protect teeth but are less durable than other fillings.
At Park 56 Dental Group, we provide personalized, quality dental care, offering pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, in a patient-centered practice with hours to fit your schedule. Schedule your complimentary consultation by contacting us online or calling (212) 826-2322.
RECENT POSTS
categories
- Uncategorized
- Cosmetic Dentistry
- Veneers
- Healthier Teeth
- Teeth Whitening
- Dental Health
- Video
- Dental Emergencies
- Invisalign
- Dental Implants
- Root Canal
- Sedation Dentistry
- Infographic
- Dental Crowns and Bridges
- Dental Anxiety
- Gum Disease
- COVID-19
- Bad Breath
- New York Dentist
- Cut out sugar
- General Dentistry
- Oral Health
- Oral Cancer
- Dry Mouth
- Gum Health
- Toothache
- Dental Sealants
- Cavities
