-
How to Prevent Gum Disease

The technical name for gum disease is periodontitis or periodontal disease. This is a common infection that, according to a recent CDC report, affects nearly half of all American adults age 30 and older.
The mildest form of this disease is called gingivitis. Early symptoms include tender and swollen gums, gums that bleed when you brush your teeth, and a receding gum line. If left untreated, periodontal disease can become painful, lead to pussy discharge, and even result in tooth loss. Advanced gum disease can also increase the risk of stroke, heart attack, and other health problems.
Protect yourself from gum disease and the associated side effects by following these preventative tips.
- Brush with fluoride toothpaste. Make this a habit every morning and evening, no matter how busy or tired you are. Use toothpaste that contains fluoride and has the ADA Seal of Acceptance. Choose a soft toothbrush, and brush thoroughly but gently to avoid irritating your gums. Brush for two full minutes, and hold your toothbrush at a 45-degree angle along the gum line so it sweeps away the bacteria hiding there.
- Floss every day. When it comes to preventing gum disease, flossing is arguably more important than brushing because it stimulates the gums and removes debris from between your teeth. The American Dental Association says it doesn’t matter when you floss—do it in the morning, at night, or after lunch—just do it!
- Swish with a medicated mouthwash. All mouthwash products offer some benefits, but some promote gum health better than others. Shop for a version that reduces plaque buildup, slows tartar formation, fights gingivitis, or all three! Remember, mouthwash complements brushing and flossing—it doesn’t replace it.
- Consider and address your risks. Some people are more likely than others to get gum disease. Risk factors include advancing age, genetics, AIDS, cancer, and hormonal changes in females. While many risk factors are out of your control, others can be addressed. For instance, you can reduce your risk if you quit smoking and control associated health conditions, such as diabetes.
- Get your teeth cleaned regularly. Gum disease develops rather quickly, and the earlier you begin treatment, the better. Therefore, children and adults of all ages should schedule a dental exam and professional cleaning every six months or as recommended by their dentist. If you already have gum disease, you may need more frequent visits to maintain your gums and prevent them from getting any worse.
At Park 56 Dental, our team of qualified dental professionals can help your smile stay healthy and beautiful. We encourage you to visit us twice a year for preventative care. Then, if you notice signs of gum disease or other oral health problems, reach out to us right away. We’ll help you slow or even reverse gum disease with effective treatments such as root planing and scaling, flap surgery, and bone and tissue grafts. Contact us online or call us at (212) 826-2322 to learn more.
-
What is a Dead Tooth?

You may not think of your teeth as being alive, but they are. The outer shell, called the enamel, is the hardest substance in the human body. However, the nerves and blood vessels at the heart of your teeth are soft and vulnerable. If this inner layer (known as the pulp) becomes damaged, blood may stop flowing. A tooth with no blood flow is called a “dead” tooth. Without treatment, this tooth may become infected or abscessed and will eventually fall out.
What Causes a Dead Tooth?
Trauma or injury is a common reason for a tooth to die. Falling or being hit in the mouth can cut off the blood supply to a tooth or even cause blood vessels to burst. With no blood flow, the nerve inside the pulp dies.
Tooth decay is another possible cause. Without consistent dental hygiene habits, cavities can start to form. Left untreated, decay slowly eats through the tooth toward the sensitive pulp, eventually causing an infection. Inflammation may cut off blood flow to the pulp, causing the tooth to die.
How to Spot a Dead Tooth
It isn’t always easy to identify a dead tooth. Only a dental professional can pinpoint signs of restricted blood flow and a dying tooth in its early stages, which is why regular dentist visits are so important. Before long, though, the problem will soon become apparent.
Pain is the first symptom to watch out for. This may seem odd because the nerve inside your tooth is dead, but that’s not where the pain comes from. Bacteria and dead nerve remnants touching the extremely sensitive nerve endings around your tooth, called the periodontal membrane, are the source of your pain.
A change in color comes next. Dead teeth often darken over time as red blood cells die. This is very similar to developing a bruise. If a single tooth in your mouth gradually becomes yellow, gray, or black, visit the dentist right away.
Signs of infection could also appear if the dead tooth doesn’t receive treatment. You may notice swelling, a bad taste in your mouth, or an inflamed sore on your gums.
Treatment for a Dead Tooth
A root canal is the first option. Dentists want to avoid removing teeth whenever possible, and this procedure could save a dead or dying tooth. It involves removing all signs of decay and infection from deep within the tooth. Then, the dentist fills and seals it. In many cases, a crown is needed following a root canal.
Tooth extraction is the next choice. Even if your dentist can’t save your tooth, prompt treatment is necessary to avoid other complications. Once removed, you have several options for replacing the missing tooth, including an implant, bridge, or partial denture.
Park 56 Dental offers tooth care and smile restorations out of our spa-like, patient-centered New York dentist office. If you notice signs of a dead tooth, please contact us online or call us at (212) 826-2322 to schedule an appointment.
-
What is a Dental Bridge?
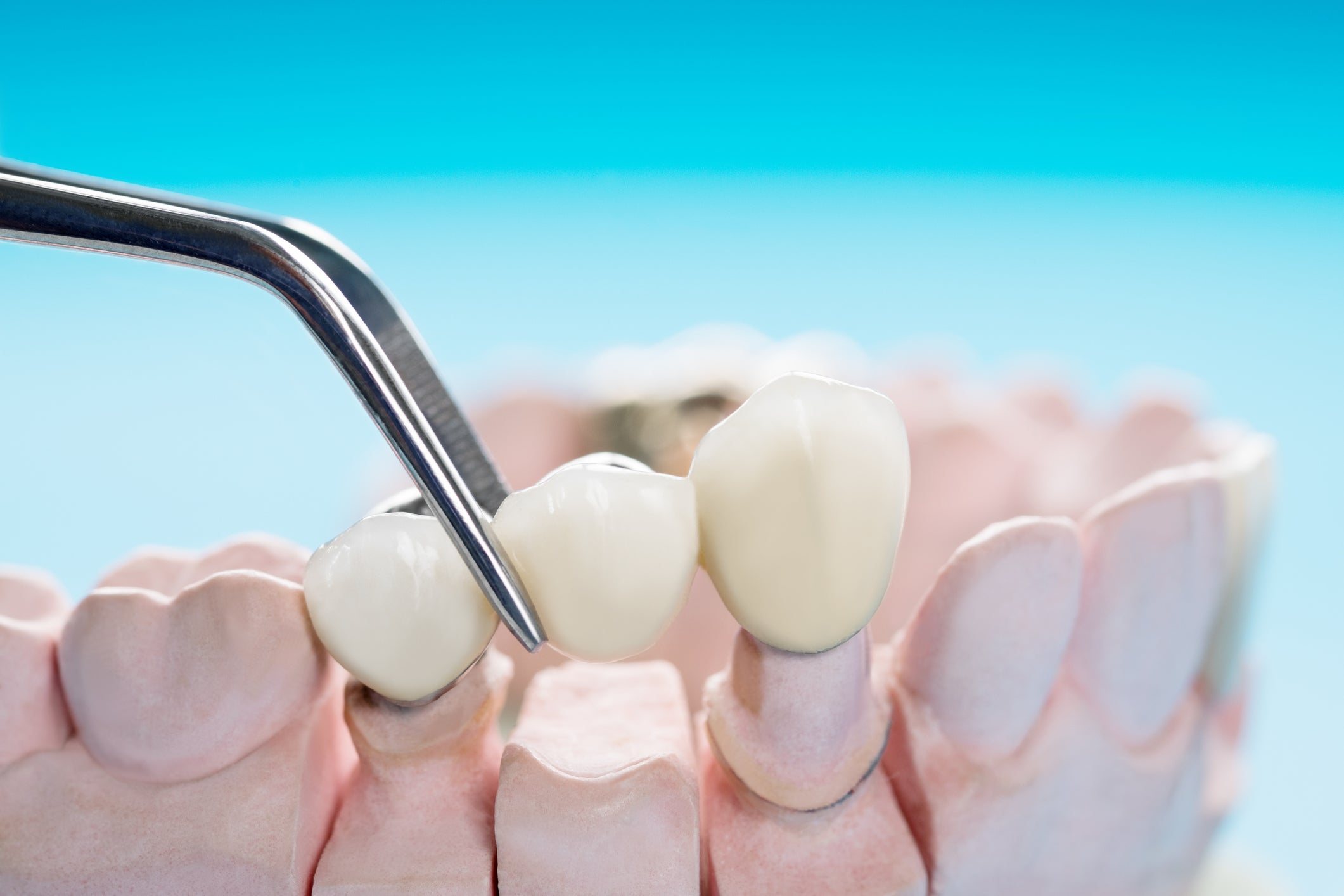
There are several options for replacing missing teeth, including dental bridges. Closing the gap in your smile can help prevent problems with your existing teeth and gums, including driting, bone loss, difficulty chewing, or speech problems. Learn more about dental bridges to help you decide if this is the right restorative treatment for you.
What is a Dental Bridge?
Dental bridges literally “bridge the gap” left by one or more missing teeth. A bridge is comprised of multiple parts:
- Crowns cap the teeth on either side of the gap, known as the abutment teeth.
- One or more false teeth, called pontics, are suspended between the crowns to replace the missing tooth or teeth.
- Crowns and pontics may be made of porcelain, alloys, gold, or other materials.
What is the Process of Receiving a Dental Bridge?
Your first visit with the dentist involves preparing the abutment teeth by removing some of the enamel. This creates room to place crowns, which serve as anchors for the pontic cemented between them.
During the same visit, your dentist takes an impression of your teeth to use as a model when creating custom pontics and crowns for your dental bridge. A temporary bridge protects your exposed teeth and gums until the permanent product is finished.
At your second appointment, the dentist removes the temporary bridge and puts the new pontic and crowns in place. Temporary cement ensures a comfortable fit. After a few weeks, you return to the dentist one final time to have the bridge firmly cemented in place.
Factors to Consider
When comparing bridges with other tooth-replacement options, keep these factors in mind:
- Time: You can complete the dental bridge process in two or three visits spaced within a few weeks of each other.
- Cost: While your insurance coverage determines what you pay out of pocket, bridges tend to be a middle-of-the-road option, with dentures costing less and implants costing more.
- Longevity: With excellent oral hygiene and regular checkups, dental bridges can last up to 15 years.
- Aesthetics: Pontics aren’t embedded in the gum line, so it may be possible to distinguish them from your natural teeth upon close inspection. For this reason, bridges often replace teeth toward the back of the mouth.
- Comfort: Bridges are not removable, so there’s no risk of slipping, which may exist with some types of dentures.
- Oral care: Whether you have a dental bridge or not, you should brush twice a day and floss once a day. If you have a bridge, your dentist may also recommend using antiseptic mouthwash and a special flossing tool to clean out debris from under the pontic.
Park 56 Dental is pleased to offer bridges and other smile restoration options to meet your diverse needs. We operate out of our spa-like, patient-centered New York office that makes going to the dentist a pleasure. Contact us online or call us at (212) 826-2322 to schedule a consultation for dental bridges in NYC today.
-
Tips to Reduce Dental Anxiety

Are you among the millions of Americans who avoid the dentist out of fear and anxiety? You might be nervous about feeling pain, being rushed to make a decision, incurring high costs, or having your concerns neglected. You might be especially prone to dental anxiety if you had a negative experience in the past.
Ironically, skipping routine cleanings could lead to oral health problems, resulting in more costly, in-depth treatment later on. Here are the top tips for reducing dental anxiety so you can take care of your smile without fear.
- Speak up: Tell your dentist about feeling anxious. It may be possible to adapt your treatment to make it more pleasant for you.
- Use hand signals: Inform your dentist that you will signal with your hands to communicate your needs. This gives you the right to raise your hand if you feel uncomfortable at any time. It’s perfectly acceptable to ask your dentist to ease off or pause the procedure.
- Focus on your breathing: If you’re nervous, you may involuntarily hold your breath. The resulting decrease in oxygen can make your anxiety worse. Close your eyes and focus on slow, regular breaths during your dental procedure.
- Listen to music: It can be helpful to shut out the world with a pair of headphones. Play your favorite album or listen to soothing songs to reduce your tension.
- Avoid caffeine and sugar before the appointment: These substances might make you even more jittery, so opt for a high-protein meal instead, which has a calming effect.
- Set a low-stress appointment time: Don’t schedule your dental visit at a time when you will feel rushed or under pressure. This might mean taking the day off work or setting a Saturday appointment so you can take your time without fear of running late.
- Try a new dentist: If your previous provider wasn’t sensitive to your needs, it might be time to find a different dentist. Ask friends and neighbors for recommendations to increase your confidence.
- Ask about sedation dentistry: Dental sedation is the best way to reduce stress for people who struggle with anxiety at the dentist. You don’t lose consciousness, but you become so relaxed that you feel completely at ease with the experience. Some patients even fall asleep in the dentist’s chair! Depending on the level of sedation you receive, you may also not remember the procedure afterward.
Park 56 Dental is pleased to help our patients overcome their fear of the dentist in our spa-like, patient-centered New York dentist office. We offer different levels of sedation to meet your needs, from inhaling nitrous oxide (laughing gas) to swallowing a pill to receiving conscious IV sedation with help from our board-certified anesthesiologist.
When you leave our office, you’ll feel so pampered—you won’t believe you once dreaded trips to the dentist! Contact us online or call us at (212) 826-2322 to learn more about our sedation dentistry options.
RECENT POSTS
categories
- Uncategorized
- Cosmetic Dentistry
- Veneers
- Healthier Teeth
- Teeth Whitening
- Dental Health
- Video
- Dental Emergencies
- Invisalign
- Dental Implants
- Root Canal
- Sedation Dentistry
- Infographic
- Dental Crowns and Bridges
- Dental Anxiety
- Gum Disease
- COVID-19
- Bad Breath
- New York Dentist
- Cut out sugar
- General Dentistry
- Oral Health
- Oral Cancer
- Dry Mouth
- Gum Health
- Toothache
- Dental Sealants
- Cavities
