-
Why it’s Important to Maintain your Gum Health
Woman flossing teeth.
Welcome to the Park 56 Dental blog, where we believe that a healthy smile starts with healthy gums! As specialists in dental care, we understand the vital role that gum health plays in maintaining overall oral health. While often overlooked, your gums provide the foundation for your teeth, ensuring they stay securely in place and function properly. In this blog post, we will be delving into why it is so crucial to prioritize gum health and the various steps you can take to keep your gums in excellent condition. No matter your age or current oral health status, we hope you find the information shared here helpful and empowering to take charge of your gum health. Let’s get started on this journey towards a vibrant and healthy smile that starts from within!
Warning Signs of Tooth Decay
Tooth decay is a common problem that results from bacteria in your mouth producing harmful acids that erode your enamel. But did you know that one of the earliest warning signs of tooth decay is actually gum problems? As the bacteria spreads, it can cause your gums to become red, swollen, and prone to bleeding. This is a sign that you should schedule a cleaning with your dentist as soon as possible.
Dental Care for Seniors: Addressing Age-specific Oral Health Challenges
As we age, our dental needs change. Seniors are more likely to suffer from gum problems due to some of these common problems/triggers:
- Dry Mouth: One of the most common oral health issues that seniors face is dry mouth. This is often caused by medications that reduce salivary flow or medical conditions such as Sjögren’s syndrome. Dry mouth can cause a range of problems, including tooth decay, gum disease, and oral infections.
- Gum Disease: Seniors are at an increased risk of developing gum disease, which is caused by a buildup of bacteria in the mouth. Gum disease can lead to tooth loss and other health problems, including heart disease and stroke.
- Tooth Loss: As we age, our teeth may begin to wear down, crack, or decay. Eventually, tooth loss may occur. Missing teeth can cause difficulty eating and speaking and may even lead to bone loss in the jaw.
- Oral Cancer: Seniors are at an increased risk of developing oral cancer, particularly if they smoke or use tobacco products. Oral cancer can be difficult to detect in its early stages, which is why it is important for seniors to receive regular oral cancer screenings.
- Medication Side Effects: Seniors may take a range of medications to manage medical conditions, and some of these medications can cause side effects that affect their oral health. For example, some medications can cause dry mouth, while others can cause gum inflammation or mouth sores.
The Hidden Dangers of Not Addressing Dental Problems
Gum disease doesn’t just affect your mouth. Studies have found that people with gum problems are more likely to develop heart disease, stroke, and other systemic conditions. This is because the bacteria that cause gum disease can enter your bloodstream and spread to other parts of your body, including your heart and lungs. That’s why it’s crucial to address gum problems early on to avoid these serious health risks.
Simple Ways to Prevent Gum Disease
Preventing gum disease doesn’t have to be difficult. By following a few simple steps, you can keep your gums healthy and your smile bright. First, make sure to brush your teeth twice a day with fluoride toothpaste. Second, floss each day to remove plaque and bacteria from between teeth and along the gumline. Finally, make sure to visit your dentist regularly for cleanings, exams, and x-rays. Taking these steps can go a long way toward avoiding gum disease and other dental problems.
Reach Out to Park 56 Dental Today with Any Questions
Keeping your gums healthy is a vital part of maintaining good oral health and avoiding serious medical problems. If you’re experiencing gum disease symptoms such as bleeding, redness or swelling, consult your dentist right away. At Park 56 Dental, we offer a full range of preventative and restorative services designed to keep your gums and teeth healthy for life. To schedule an appointment, call us at (212) 826-2322 today.
-
Tips and Advice for Flossing in Recognition of National Flossing Day

Man taking care of teeth by making sure to floss.
National Flossing Day is right around the corner, and whereas it might be slightly overshadowed by Thanksgiving and Native American Heritage Day, it’s still a great time to give three cheers for the unsung hero of dental hygiene, the modest waxed string we know as dental floss.
Why Should You Floss?
Most of the daily emphasis on toothcare is on brushing, which removes bacteria, food, and grime from the surface of the teeth. But where flossing truly shines is in getting into those hard-to-reach spaces in between teeth and close to the gum line, where regular toothbrushes can’t reach. Flossing helps fight gingivitis and periodontitis, reducing the risk of gum inflammation and cavities. Flossing also helps promote fresh breath by removing the food and bacteria that collects between your teeth.
Tips for Effective Flossing
- Choose the Right Floss:
- There are various types of dental floss available, including waxed, unwaxed, flavored, and wider tape-style floss. Choose the one that feels most comfortable and effective for you.
- Establish a Routine:
Make flossing a daily habit. Aim to floss at least once a day, ideally before bedtime, to remove accumulated plaque and food particles.
- Proper Technique:
-
- Start with an 18-inch (45 cm) length of floss. Wind most of it around one finger on each hand, leaving about 1-2 inches (2-5 cm) of floss to work with.
-
- Gently slide the floss between your teeth using a sawing motion. Avoid snapping it into place, which can harm your gums.
-
- Curve the floss around the base of each tooth, forming a C-shape, and gently glide it up and down. Be gentle to avoid damaging your gums.
-
- Use a fresh section of floss for each tooth to avoid transferring bacteria.
- Be Patient:
-
- Take your time when flossing to ensure thorough cleaning. Rushing can lead to incomplete removal of plaque and debris.
- Keep Flossing Agents Handy:
- Keep floss in your purse, briefcase, backpack or satchel. Floss picks are also a convenient minimal device for a quick cleaning when out and about.
- Use Flossing Aids:
-
- If traditional flossing is challenging, consider using floss picks, interdental brushes, or water flossers. These tools can make the process more accessible and convenient.
- Teach Children Early:
-
- Encourage good oral hygiene habits in children by teaching them to floss as soon as part of your family culture. Child-friendly floss and flossers are available.
- Avoid “Bleeding Gums” as an Excuse:
-
- If your gums bleed when you first start flossing or after a break, don’t be discouraged. This is a sign of gum inflammation and indicates the need for regular flossing to improve gum health.
- Set Reminders:
-
- Use phone alarms or other reminders to ensure you don’t forget to floss daily, especially if you’re establishing a new habit.
Call Park 56 Dentistry to Celebrate
Our dental professionals are always available to celebrate National Flossing Day with you, to help you analyze your flossing technique, or to offer advice on the best type of floss for you. November is also a great time to contact us and schedule your end-of-year cleaning or get on the schedule after the new year.
-
How Chronic Illnesses Can Affect Oral Health
 Woman taking care of dental health by brushing teeth.
Woman taking care of dental health by brushing teeth.Oral Health and Overall Health
Did you know that the health of your mouth and the overall health of your body are connected? In fact, there is a bidirectional relationship between chronic illness and oral health. Some chronic diseases are directly associated with oral health issues, either causing or being caused by them. In other cases, there’s an indirect relationship, or shared risk factors. Let’s take a look at how chronic illnesses can affect oral health.
Chronic Diseases are Leading Causes of Death and Disability
Conditions like diabetes, heart disease, respiratory disease, cancers, and obesity can all be linked with poor oral health. Because oral health conditions are often chronic, they can happen alongside other chronic conditions. Unfortunately, people with more than one chronic condition tend to have worse long-term health outcomes than those who only have one chronic condition. Prevention is the key to good health, and maintaining good oral health care can help prevent chronic diseases or improve the outcome for those who suffer from them.
Preventing Gum Disease Can Improve Health
Gum disease is very common, affecting about 75 percent of adults in the United States. If left untreated, gum disease can advance and increase the risk of serious health issues, like diabetes, heart disease/stroke, lupus, oral cancer, organ transplant, and rheumatoid arthritis. Fortunately, when detected early, gum disease can be reversed through good oral hygiene and regular dental care.
How Different Conditions are Connected
- Diabetes, periodontal disease, and tooth decay are interconnected. Though more research is needed, there is evidence to suggest that periodontal disease and tooth decay can exacerbate type 2 and gestational diabetes. This probably occurs because these conditions increase inflammation and blood sugar levels. By the same token, people who have diabetes are at higher risk of infections that can cause tooth decay and periodontal disease.
- Oral health issues may be associated with heart disease. Studies show that periodontal disease and tooth decay may increase a person’s risk of heart disease, or worsen existing heart conditions, by causing inflammation and damaging blood vessels.
- Tooth decay and periodontal disease may be associated with respiratory disease. There are studies that suggest that by causing an increase in bacteria, periodontal disease and tooth decay can increase the risk of respiratory conditions, including emphysema, pneumonia, and COPD, due to bacteria from the mouth colonizing in the respiratory tract. People at highest risk include older people, those who wear dentures, and people with decreased immune system function.
- Periodontal disease and tooth decay may be linked to some cancers. Even after controlling for other risk factors, like smoking and diet, there is evidence to suggest that oral health problems may be connected to cancers like lung, pancreatic, and head/neck cancers. In one study, a 35 percent increased risk for blood cancer and 21 percent increased risk for cancer in general for men with periodontal disease, and another suggests that there is also a 63 percent increased risk of pancreatic cancer. Still another study suggests a 43 percent higher risk of esophageal cancer and a 52 percent higher risk of stomach cancer for those with periodontal disease, as compared to people with healthy gums.
- Obesity may increase the risk of oral health issues. The result of preliminary research on obesity and oral health speculates that secretions from adipose tissue increase the risk of inflammation, decreasing immunity as well as blood flow to the gums.
Talk to Your Dentist About Your Medications
Sometimes, the drugs prescribed for chronic illnesses can cause side effects that impact their oral health. For instance, swollen and bleeding gums, along with dry mouth can be side effects of medications for hypertension and heart conditions. Some drugs for high blood pressure can cause gum overgrowth, which can lead to decay and progressive gum disease. Because inflamed gums bleed easily, there is also a risk for ulceration and soreness. Other medications for hypertension can reduce saliva production, putting patients at risk for dry mouth and tooth decay. Heart medications like anticoagulants and blood thinners can raise a patient’s risk for prolonged bleeding, and can cause gums to bleed during brushing. There is also a risk, with these medications, of post-extraction bleeding or bleeding during cleaning. Your dentist might want to talk to your doctor about changing your medication.
Partner with Park 56 for a Healthy Mouth
If you’re looking for a dentist in New York, why not choose the dentist voted best in the city? At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Why Your Gum Line Recedes
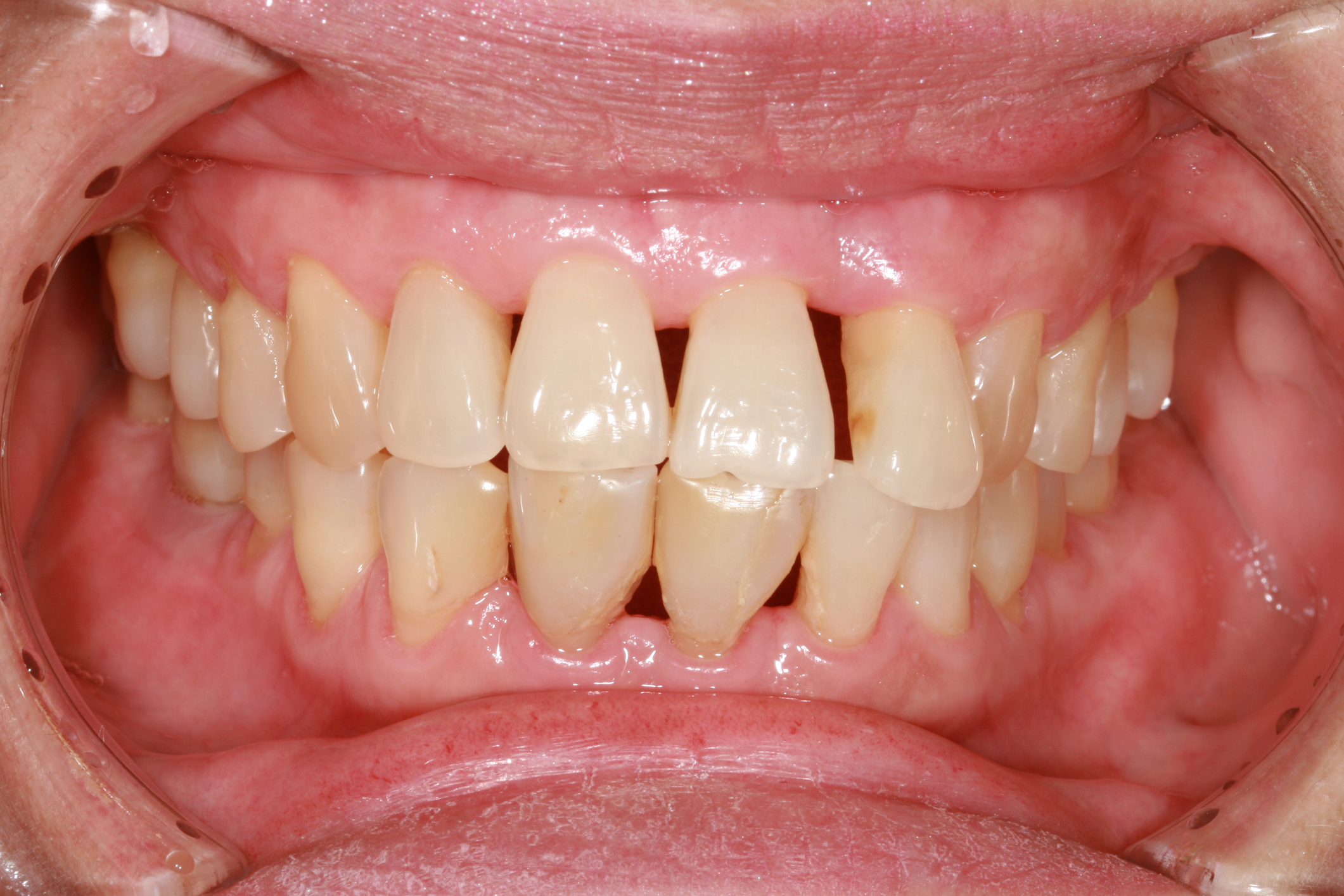
Gum recession.
How is your gum health? About half of all people over 30 suffer from periodontal disease, and this is the leading cause of gum recession. Gum recession is a problem, because when your gums recede too far, they can allow your teeth to fall out! Further, receding gums create pockets between the teeth and gums, and this can allow bacteria to grow and cause infections. In this way, even if your gum recession is not caused by periodontal disease, it can create an ideal environment for periodontal disease to progress. Once gums have receded, they don’t grow back, but there are some strategies you can employ to slow the recession. First, you need to know what is causing your gum line to recede.
- As mentioned, periodontal disease is a major cause of receding gums. The bacterial gum infections of periodontal disease can destroy not only gum tissue, but also the bone that holds the teeth in place. Catching periodontal disease in the early stage, called gingivitis, when the gums are simply inflamed, can help forestall its progression.
- It could be your genes. Sometimes, genetics just don’t work in your favor when it comes to your gums. About 30 percent of people have receding gums, leading to periodontal disease, no matter how well they care for their teeth.
- You might not be taking good care of your teeth. Poor oral hygiene can lead to tartar build-up, and when this happens, it can cause your gums to recede.
- On the other hand, you might be brushing too enthusiastically. Aggressive brushing can wear away your enamel and damage your gum tissue.
- Your teeth may be crooked. Believe it or not, misaligned teeth can wear on your gums. Teeth that don’t come together properly put too much force on the gums, causing them to recede.
- It might be hormones. Hormonal fluctuations, like the ones experienced during puberty, pregnancy, or menopause, can cause your gums to recede.
- Mouth trauma can damage your gums. If you get punched in the mouth or fall on your face, your teeth can be knocked loose, and your gums can sustain damage that causes recession.
- Your orthodontia may be the issue. It makes sense that using constant force to reposition your teeth could cause your gums to become inflamed and recede.
- If you grind your teeth, your gums might recede. In fact, receding gums may be your first warning sign that you grind your teeth at night.
- Tobacco use can lead to receding gums. Smoking and chewing tobacco are bad for your oral health in such a variety of ways that if you use tobacco, you really need to stop.
You might notice your gums receding, or you might notice some other warning signs. Your teeth may become sensitive to heat, cold, and sweets, or they may be sensitive when you’re brushing, flossing, or getting dental cleanings. You may also experience pain or discomfort near the gum line. Without treatment, gum recession could cause your teeth to feel loose. Fortunately, while receding gums won’t grow back, your dentist can help you slow the recession, as well as offering non-surgical and surgical treatments to improve the condition.
When you’re looking for a dentist to help with your teeth and gums, trust the dentist voted best in New York. At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Reasons Why your Teeth are Temperature Sensitive

Do you find that eating ice cream or drinking hot coffee causes pain in your teeth? You may have sensitive teeth. It’s a common condition, affecting about 45 million people in the United States, but it can be painful and difficult. What causes teeth to be temperature sensitive? More importantly, what can be done about it?
Your dentist can help you determine the underlying cause of the sensitivity, though the reason teeth become sensitive is typically always the same. Teeth are made of three layers, the enamel, the dentin, and the pulp. The enamel is the hard, outer layer of the teeth, and it protects the softer, inner layers. Below the enamel is the dentin, which is made up of microscopic tubes leading to the innermost layer- the pulp. Within that pulp is the nerve system of the teeth, and dental sensitivity happens when the dentin layers or the nerves are stimulated by something hot or cold. The cause of this stimulation varies.
Cold sensitivity can be caused by tooth decay or gum disease. It can also be the result of brushing too aggressively, using abrasive toothpaste, or using a hard-bristled toothbrush, which can all wear away at the enamel. Tooth grinding or clenching can chip the teeth or damage tooth enamel, which can also cause sensitivity to cold. Receding gums and cracks in a tooth can leave that tooth vulnerable to the cold. If your teeth are sensitive to heat, though, it could have a different cause. Dental treatments like teeth whitening can lead to heat sensitivity, and so can teeth cleanings, root planning, and dental crown or filling placement. If you consume a diet that’s high in acids, found in foods like coffee, tomato sauce, and wine, it can lead to enamel loss and heat sensitivity. People struggling with gum disease often have sensitive teeth, because 80 percent of tooth sensitivity begins at the gum line.
If your teeth are highly sensitive and react to both heat and cold, the best thing to do is see a dentist to determine the cause and the best course of treatment. If the sensitivity is minor, though, you may be able to manage it at home. You can reduce the discomfort of mild temperature sensitivity by making a few changes.
- Instead of letting hot and cold liquids touch your teeth, use a straw.
- Reduce your consumption of acidic foods.
- Change to a softer bristled brush and be careful not to brush too hard.
- Switch to a toothpaste for sensitive teeth.
- Ask your dentist which mouthwash to use; some mouthwashes can irritate your dentin and pulp layers.
- Wear a mouthguard to prevent teeth grinding at night.
There are also treatments that dentists offer to improve dental sensitivity. If you find that your sensitivity is not improving after a few days, talk to your dentist about the best treatment for you. It could be as simple as fluoride therapy, or it could be a more involved procedure like a root canal or a gum graft. Dental restorations like a filling, inlay, onlay or crown can also protect damaged teeth and help with sensitivity. Nervous about seeing the dentist? We provide sedation dentistry for your comfort.
If you are looking for a dentist to help with tooth sensitivity, it makes sense to choose the practice voted Best in New York. At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322.
-
Understanding Your Gums
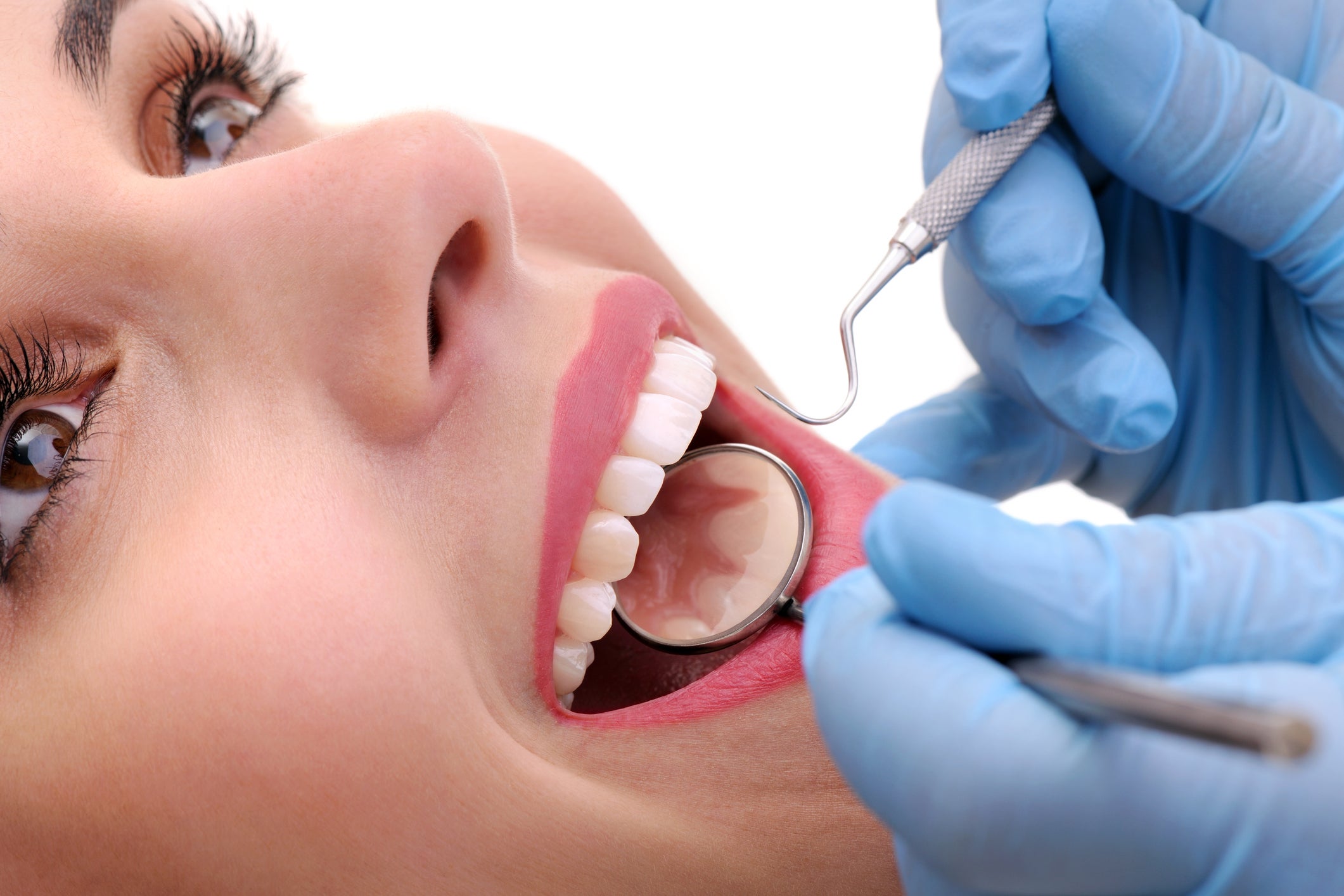
You know about cavities, and tooth decay, and how important it is to brush and keep your teeth healthy. But how much do you know about the health of your gums? The gums are an important part of your mouth, and if they’re not in good shape, your whole mouth can suffer. What do you need to know about your gums?
You might have noticed that your oral hygienist or dentist probes your gums during your regular check-ups. This is to determine if your gums are fitting snugly against your teeth. Unhealthy gums have pockets of space, and the deeper the pocket, the worse your gum health. It may feel like your gums are just being poked, but what the dentist is actually doing is measuring them. The tool used to probe gums is called a periodontal probe, and it’s essentially a tiny ruler. It is inserted into pockets in your gums, and the depth is recorded in millimeters.
Your dentist will keep track of these numbers as a preventive measure against periodontal disease (gum disease). Only your dentist can diagnose gum disease, but in general, 1 to 3 mm means the gums are generally healthy, 4 mm means you need to pay more attention to your oral care, 5 to 6 mm indicates gum disease, and anything over 6 means advanced gym disease. By regularly checking gum pocket depth, your dental team can catch periodontal disease early, when it’s still relatively easy to treat.
You can look for signs of gum disease at home, too. Swollen, sore, or bleeding gums could be a sign of gingivitis or periodontal disease. Gingivitis is the early stage of gum disease, and it happens when plaque builds up at the gumline. Once it progresses to periodontitis, it can affect the bone and tissue supporting your teeth. However, these symptoms can also be caused by other conditions and even vitamin deficiencies. Hormonal changes like pregnancy, illnesses like diabetes, infections, and vitamin C deficiency can all be responsible for gum problems, so you will want to see your dentist to get the right diagnosis.
What can you do to keep your gums healthy? First, pay attention to your oral care routine. Brush twice a day and floss once a day, brushing gently so that you don’t injure your gums. Consider using a water flosser, to clean below the gumline. Eat a nutritious diet, don’t use tobacco products, drink alcohol only in moderation, and take supplements, especially if you think you are not getting enough vitamin C. See your dentist for regular check-ups and cleanings, but in between visits, pay attention to your gums so that you can make a dental appointment if you notice signs of gum disease.
At Park 56 Dental Group, we offer pediatric, prosthodontics, endodontics, oral surgery, Invisalign®, emergency, and sedation dentistry, all at the highest level of treatment. We serve the Midtown, Central Park, Upper East Side, Park Avenue, and all surrounding Manhattan and New York areas, with a patient-centered practice that has hours to fit your schedule. Schedule your complimentary consultation today by contacting us online or calling us at (212) 826-2322
-
Why Your Gums Itch

You know that feeling when your gums start to itch? The sensation can be annoying, and it might even make you a little self-conscious. But did you know that gum itchiness is actually a sign of something else going on in your mouth? There are a few different things that can cause your gums to itch. Read on to learn more about common causes of itchy gums and what you can do about it!
What Causes Gums to Itch and What Are Symptoms?
The most common cause of itchy gums is plaque build-up. Plaque is a sticky film of bacteria that forms on your teeth and gums. When plaque isn’t removed, it can harden into tartar. Tartar can irritate your gums and cause them to itch. Other causes of itchy gums include:
- Gum disease – Gum disease is an infection of the gum tissue. It can cause swelling, redness, and bleeding of the gums.
- Allergies – Allergies to food, medication, or other substances can cause itching and swelling of the gums.
- Dry mouth – Dry mouth can occur due to certain medications, medical conditions, or treatments. It can cause the gums to become irritated and itch.
Symptoms of itchy gums include:
- itching
- redness
- swelling
- tenderness
- bleeding
Are Itchy Gums a Warning Sign for a More Serious Issue?
Itchy gums are usually not a sign of a more serious condition. However, in rare cases, they may be a sign of gum disease or another oral health problem. If you have any concerns, see your dentist or oral healthcare provider.
What Are My Options for Treatment and Relief?
The best way to treat itchy gums is to remove the plaque and tartar with professional dental cleanings. Your dentist or oral healthcare provider can also recommend other treatments, such as:
- Fluoride mouth rinse – This can help prevent plaque build-up.
- Soft toothbrush – A soft-bristled toothbrush can be less irritating to your gums.
- Medications – If your itchy gums are caused by an allergy, your doctor may prescribe medication.
When Should I See a Doctor for My Itching Gums?
You should see a dentist or oral healthcare provider if your itchy gums are severe or don’t improve with home treatment. You should also see a healthcare provider if you have any other symptoms, such as:
- fever
- swelling of the face or lips
- difficulty breathing
How Can I Prevent Itchy Gums?
You can help prevent itchy gums by practicing good oral hygiene. This includes brushing your teeth twice a day, flossing daily, and using a fluoride mouth rinse. You should also see your dentist regularly for professional dental cleanings and check-ups.
How Can Park 56 Dental in NYC Help Me Treat My Itchy Gums?
If you have itchy gums, the team at Park 56 Dental in New York can help. We offer professional dental cleanings and a variety of other treatments to help relieve your symptoms. We also offer preventative care services to help you avoid itchy gums in the future. To learn more, contact us today or schedule an appointment online.
RECENT POSTS
categories
- Uncategorized
- Cosmetic Dentistry
- Veneers
- Healthier Teeth
- Teeth Whitening
- Dental Health
- Video
- Dental Emergencies
- Invisalign
- Dental Implants
- Root Canal
- Sedation Dentistry
- Infographic
- Dental Crowns and Bridges
- Dental Anxiety
- Gum Disease
- COVID-19
- Bad Breath
- New York Dentist
- Cut out sugar
- General Dentistry
- Oral Health
- Oral Cancer
- Dry Mouth
- Gum Health
- Toothache
- Dental Sealants
- Cavities
